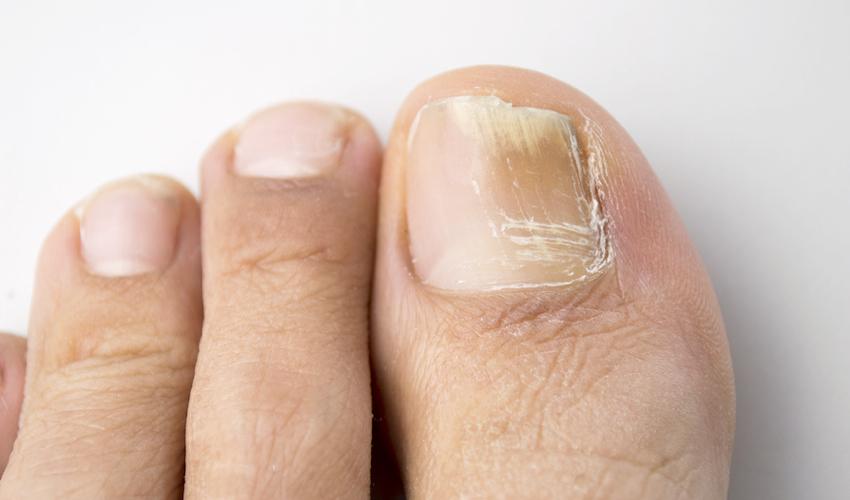
Many people develop a fungal nail infection at some point in their life (1 in 4 people are infected at any given time), and although it is not usually serious they can be cosmetically unattractive, cause pain and can be difficult to treat.
Infection develops slowly and can cause the nail to become discoloured, detached from the nail bed, brittle or crumbly, thickened and distorted. The nails can be difficult to cut, can cause pain when pressed against footwear and sometimes the skin surrounding the nail may also become infected and be itchy, cracked, red and swollen. Toenails are more frequently affected than the fingernails and are more difficult to treat.
Causes & Prevention of Fungal Nail Infections
Fungi often live harmlessly on your skin, but they can sometimes multiply and lead to infections.
The fungi responsible is usually the one that causes athlete’s foot which then spreads to the nails or nail bed. Fungal nail infections are generally more likely to develop when your feet are frequently warm and damp, in the elderly, if you have a weakened immune system or certain other health conditions such as diabetes, psoriasis or poor peripheral circulation.
To help prevent fungal nail infections:
| DO | DONT |
| ✔ keep your feet clean and dry | X wear shoes that make your feet hot and sweaty |
| ✔ wear clean socks every day | X wear other people’s footwear |
| ✔ wear well-fitting shoes made of natural materials | X walk barefoot in communal areas |
| ✔ alternate shoes to allow them to dry out naturally | X share towels |
| ✔ treat foot infections such as athlete’s foot as soon as possible to avoid spread to nails | X share nail clippers or nail scissors |
| ✔ replace old footwear that may be contaminated with fungi | X use nail/beauty salons that don’t use single use items or adequately sterilise equipment between uses |
What Are The Treatments For Fungal Nail Infections?
Fungal nail infections can be successfully cured but are difficult to treat, will require persevering with treatment for up to a year and they annoyingly commonly reoccur.
Good foot hygiene should be practiced to reduce the risk of the infection spreading to other nails, to other parts of the body or to other people. These nail infections do not clear up by themselves, but as some people are not bothered by them not all infections need treating.
Speak to your podiatrist, GP or pharmacist if you are bothered by the appearance of affected nails, or if they are causing problems such as discomfort.
There are different treatment options which can be discussed with you and sometimes a nail sample may be needed to be sent to a laboratory to confirm diagnosis of a fungal infection (could also be due to yeast or mold infection):
- Antifungal nail paints: do not work as well as oral tablets. They are more likely to be effective if the infection is treated at an early stage, but the cure rate is quite low, approximately 15-30%. The treatment is applied directly on top of the nail over a period of several months.
- Nail softening creams: applied for about 2 weeks to soften the nail which is then scraped off.
- Anti-fungal tablets: prescribed by your GP (if there are no contraindications) and taken for up to 12 months depending which tablets are prescribed. These tablets can’t be taken if you are pregnant or have certain medical conditions. Some oral treatment option may be suitable for children and blood tests may have to be taken to check your liver function. Success rates are variable but may only be up to 50%. If oral treatment is being considered for children, they should be referred to a dermatologist – as your GP to refer.
- Total nail removal: a mini surgical procedure done by a podiatrist, after numbing the toe with a local anaesthetic.
- Laser treatment: a light-energy laser is projected and absorbed by the targeted area, producing heat and destroying the fungus. Medical lasers are expensive devices and so treatments are often quite expensive and not available on the NHS so you would have to see a private practitioner. Laser therapy for the treatment of fungal nails is quite new, so data is still limited to support the efficacy of this medical treatment option.
- Alternative or natural products: You may hear about other treatment options such as tea tree oil, vinegar, Vicks or urine. There is no strong clinical research evidence to suggest that these are safe or effective and should therefore not be advised as a treatment option by a health professional. Tea tree oil is a volatile essential oil that can cause dermatitis and allergic responses and is actually classified as a Schedule 6 Poison in Australia. Vicks is registered for use as a decongestant only. It contains volatile essential oils that produce peroxides and should not be used on broken or damaged skin. Fungal nail infections do damage the skin as the dermatophytes cause a breach in the epidermis (top layer of the skin).